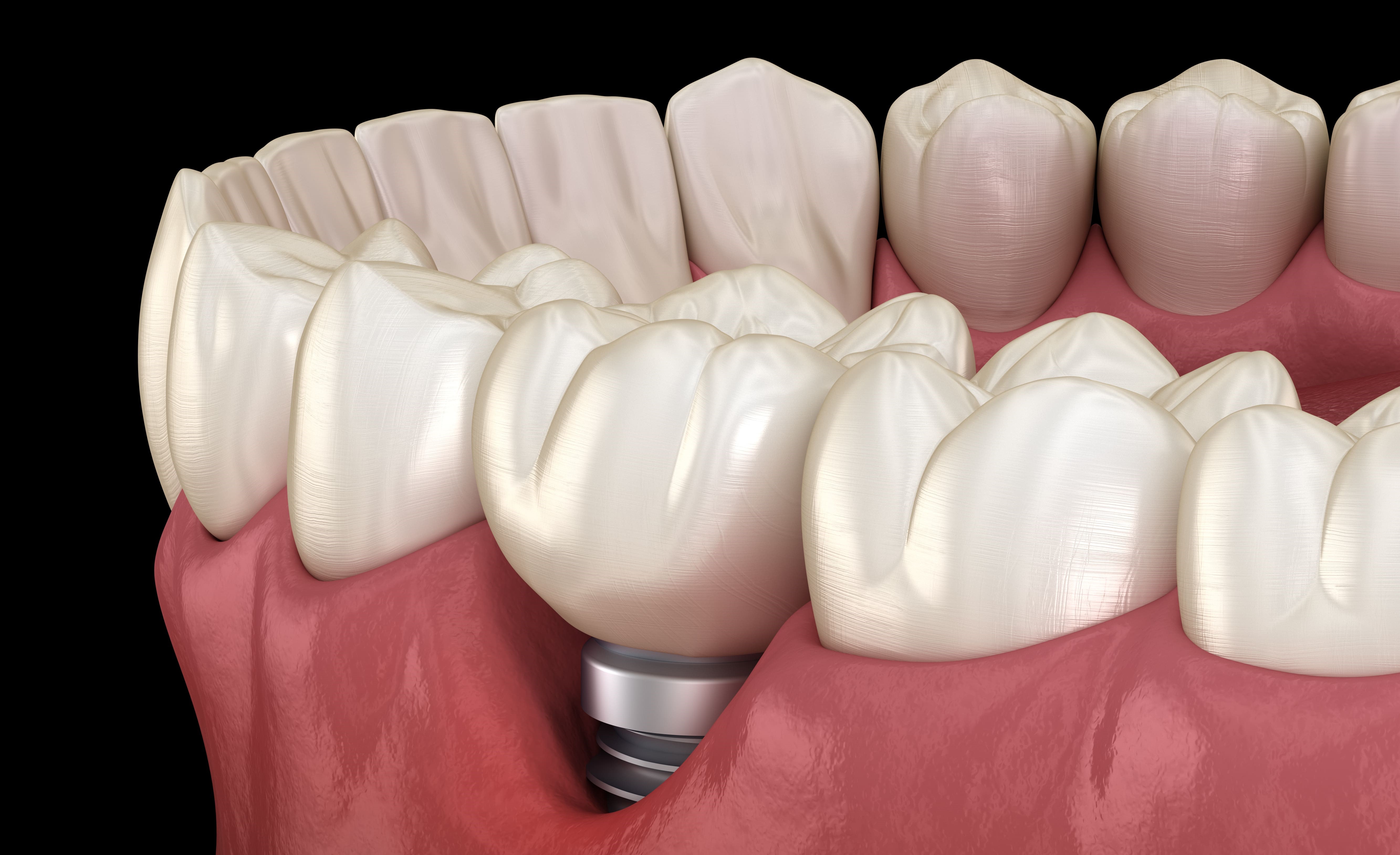
Further to the anatomical-histological review of periodontal and peri-implant tissues, this second part will focus on epidemiological data, the various means of diagnosis and the different risk factors.
Epidemiological data
In the absence of a consensus on peri-implantitis, and taking into account the different selection criteria from one study to another (e.g. pocket depth and degree of bone loss), the figures published in this article may underestimate the true incidence and prevalence of peri-implantitis.
Implant success rates range from 95-98% but do not prejudge the medium to long term outcome of an implant.
In 2008, the European Workshop on Periodontology (EWOP) published the results of two studies conducted on 662 patients (i.e. 3,413 implants) and 216 patients (i.e. 987 implants). The first study concluded the prevalence of peri-implantitis in 27.8% of patients and 2.4% of implants, while the Panos N et al study concluded its prevalence in 34% of patients and 21% of implants.
A disparity in results can be observed due to both the absence of studies on peri-implantitis and the lack of international consensus on how it can be diagnosed. Despite this, the prevalence rate of peri-implantitis is significant, so it is important to know how to diagnose it. Peri-implantitis can be detected in a number of ways.
Diagnosis of peri-implantitis
A peri-implant survey
This is a reliable method for diagnosing and evaluating the depth of peri-implant pockets.
The periodontal probe is an essential tool, which must be handled with care in order to avoid distorting the probing results. In the case of healthy tissue, the tip of the periodontal probe penetrates the sulcus to probe its depth. In the case of inflammation, the tissue is softer and the pockets may appear deeper than they really are. Bleeding on probing is a characteristic sign of peri-implant tissue inflammation.
Probing greater than or equal to 5mm suggests that peri-implantitis has set in (to be verified through further examinations).
Radiological assessment
Panoramic radiography and intraoral radiography using parallel long cones have been widely employed to assess the level of marginal bone.
A panoramic radiograph allows the entire implant to be visualised. This technique is widely used despite its limitations – it is unreliable for assessing lingual and palatal bone loss. Other more efficient methods, such as three-dimensional radiographs, exist but are less used in current practice.
Mobility of the implant
This indicates an absence of osseointegration, in which case the implant must be removed. Mobility is therefore useless for an early diagnosis of peri-implant disease.
In order to better prevent peri-implantitis, it is vital to be aware of the factors that can cause it.
Risk factors
A patient is more likely to develop peri-implantitis if he or she has a history of…
Periodontitis
A patient with a history of periodontitis is considered more likely to develop peri-implantitis: according to Meyle et al, the chances are two to three times higher.
Smoking
Patients who smoke tend to develop peri-implantitis more quickly than non-smokers. Meyle et al found that a patient who smokes has a 2.25 times higher risk of losing a functional implant than a non-smoking patient. They also add that bone grafts are less successful in smokers.
Occlusal trauma
Excessive occlusal loading is one of the major determinants of implant loss. Esposito et al reported that occlusal overloads are a major contributor to the development of peri-implantitis.
Poor oral hygiene
Plaque is the most important etiological factor in peri-implantitis.
Certain pathological conditions
These include the use of long term non-steroidal anti-inflammatory drugs, bisphosphonate therapy, unbalanced diabetes, or radiation therapy in the case of certain head and neck cancers.
Key points to remember
- Peri-implantitis is an inflammation of the peri-implant tissues associated with a loss of the implant’s supporting tissues. It is microbial in origin.
- Peri-implantitis is often the cause of dental implant loss.
- Knowledge of the factors favouring the development of peri-implantitis can help the practitioner prevent it.
- It is essential to educate patients who smoke to stop smoking permanently to better promote osseointegration.

Saïd BOUTOUGHMAS
Dentist and quality and regulatory affairs officer at HYGITECH.
Sources
Meyle J, Casado P, Fourmousis I, Kumar P, Quirynen M, Salvi GE.
General genetic and acquired risk factors, and prevalence of peri-implant diseases – Consensus report of working group 1. Int Dent J. 2019 Sep;69 Suppl 2:3‑6.
Naveau A, Shinmyouzu K, Moore C, Avivi-Arber L, Jokerst J, Koka S.
Etiology and Measurement of Peri-Implant Crestal Bone Loss (CBL). J Clin Med. Feb 2019; 8(2): 166.